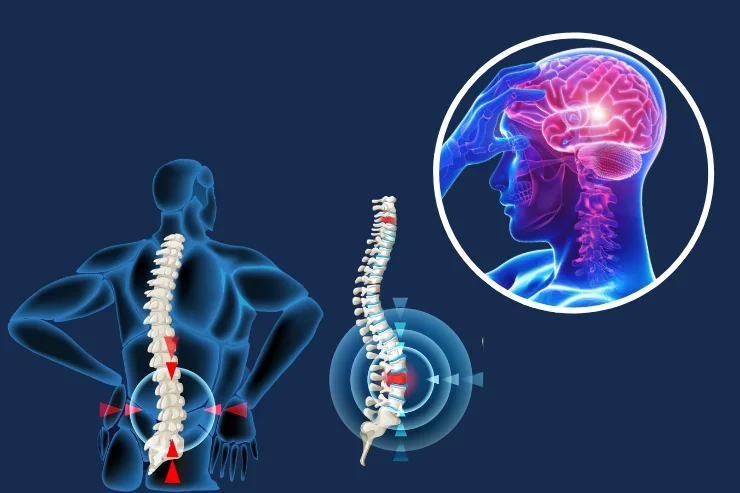
Lumbar and neck hernia is a condition in which the pads (discs) between the bones (vertebrae) that make up the spine are damaged and the gelatinous substance inside leaks out and puts pressure on the nerves.
This is a mechanical and chemical process that can lead not only to regional pain, but also to loss of strength, numbness and severe functional limitations in the arms and legs reached by the nerves.
What is a Herniated Disc?
Lumbar Disc Herniation, medically known as Lumbar Disc Herniation, is the disruption of the integrity of the disc structure between the vertebrae in the lumbar region and its protrusion into the nerve canal.
Herniated disc usually occurs as a result of intense mechanical load in the lower lumbar region (L4-L5 or L5-S1) and compresses the nerve roots leading to the legs, triggering conditions such as sciatica pain.
According to Assoc. Prof. Dr. Erdinç Özek; “It is wrong to think that every patient diagnosed with herniated disc should undergo surgery. The important thing is not the size of the hernia on the MRI image, but the findings in the patient’s neurological examination and the decline in the quality of life.”
What are the Symptoms of Herniated Disc?
The clinical picture of a herniated disc varies depending on the level of the hernia and the severity of the pressure on the nerve.
- Severe Low Back and Leg Pain: Sharp pain that is usually unilateral and extends from the buttocks to the feet.
- Numbness and Tingling: Loss of sensation that spreads to the toes.
- Muscle Weakness: Motor losses such as inability to pull the ankle up (drop foot) or inability to stand on tiptoe.
- Reflex Losses: Decrease or disappearance of the knee or Achilles reflex.
- Advanced Signals: Loss of urinary and fecal control, which is a rare but emergency condition (Cauda Equina Syndrome).
Causes of Herniated Disc
Aging of the spinal discs and loss of fluid content (degeneration) is the main risk factor.
- Aging and Wear: Discs lose their elasticity and rupture more easily.
- Heavy Lifting and Incorrect Movements: Sudden strains that are contrary to body mechanics.
- Obesity: The static load on the spine disrupts the structure of the discs.
- Sedentary Life: As a result of the weakening of the waist muscles, the load is completely on the discs.
- Genetic Predisposition: Having a family history of disc herniation.
What is Neck Hernia?
Neck hernia, called Cervical Disc Herniation, is when the outer layer of the discs between the seven vertebrae in the neck region ruptures and the inner part presses on the nerve roots or spinal cord.
Since neck hernia occurs in a narrower canal than lumbar hernia, it may carry a direct risk of spinal cord compression (myelopathy) and this requires more sensitive follow-up.
What are the Symptoms of Neck Hernia?
In neck hernia, pain is not only trapped in the neck; It is reflected in the arms and hands along the nerve trace.
- Pain radiating from the neck to the arm: A feeling of electrification that usually starts over the shoulder and goes down to the fingertips.
- Loss of Strength in Hand and Arm: Difficulty holding objects, slowing down in hand skills (buttoning, etc.).
- Sensory Loss: Numbness in the hands, tingling and sometimes inability to distinguish between hot and cold.
- Limitation in Neck Movements: Increased pain and stiffness when turning the neck to the right or left.
Causes of Neck Hernia
Posture disorders brought about by modern life have caused a serious increase in neck hernia cases.
- Posture Disorders (Text Neck): Keeping the neck tilted forward for a long time while using a smartphone and computer.
- Sudden Traumas: Whiplash in traffic accidents or sports injuries.
- Neck Calcification: Narrowing of disc distances due to age.
- Occupational Factors: Overloading the drives in desk workers or overhead workers.
Clinical Experience Note (Anonymous Case): In a 35-year-old patient who was constantly working at the computer, the process that started with only mild neck pain turned into difficulty holding a pencil in his right hand over time. In the examinations, it was seen that the hernia directly pressed on the nerve root; With the right ergonomic arrangements and microsurgical planning, the patient’s fine motor skills were completely preserved.
Waist and Neck Hernia Diagnostic Methods
The most critical stage in the diagnosis of hernia is to determine whether the patient’s complaints and radiological findings coincide with each other.
The diagnostic process begins with a detailed physical and neurological examination performed by a specialist physician; muscle strength, reflexes and sensory tests are performed.
- MRI (Magnetic Resonance): It is the gold standard method that most clearly shows soft tissues, the condition of the discs and nerve pressure.
- CT (Computed Tomography): It is mostly preferred to examine changes in bone structure and calcifications.
- EMG (Electromyography): By measuring the electrical conduction of nerves, it embodies which nerve root and to what extent the damage is located.
Waist and Neck Hernia Treatment Options
Today, hernia treatment is managed with a “minimally invasive” approach that aims to restore the patient’s health with minimal surgical trauma.
When making a treatment decision, the type of hernia, the degree of pressure on the nerve and the patient’s existing neurological losses (such as loss of strength) are taken into consideration.
Non-Surgical Treatment Methods (Conservative Treatment)
Approximately 90% of hernia patients can recover with properly planned conservative treatments without the need for surgical procedures.
Medication and Rest
In the acute period, painkillers and muscle relaxants are used to control pain and reduce edema (inflammation) in the nerve.
However, instead of long-term bed rest, it is more recommended in modern medicine that the patient switches to controlled mobility after the first few days of rest.
Physical Therapy and Rehabilitation
It is aimed to strengthen the muscles and reduce the load on the spine. The pressure on the disc is tried to be balanced with manual therapy, traction and special exercise programs.
Injection Treatments
In cases where the pain is very severe, injections of steroids and local anesthetics into the nerve root or epidural area (pinpoint therapy) can quickly calm the inflammation.
Surgical Treatment Methods
Surgery is performed only in cases where non-surgical methods do not respond or when the patient develops neurological emergencies such as severe loss of strength and urinary incontinence.
Microsurgery Method
Microsurgery is the most widely used reliable surgical method using an operating microscope, which causes the least damage to nerve tissue.
By entering through a very small skin incision, only the herniated tissue is cleaned and healthy nerve structures are preserved thanks to the high magnification and depth perception provided by the microscope.
Fully Closed (Endoscopic) Waist and Neck Hernia Surgery
Endoscopic surgery is the most advanced stage of hernia surgeries. It is performed by entering with a camera through a single hole of approximately 0.5 cm.
Tissue damage is almost non-existent; This means that postoperative pain is minimal and the patient can stand up on the same day.
| Feature | Microsurgery | Endoscopic Surgery |
| Incision Size | 1.5 – 2 cm | 0.5 – 0.7 cm |
| Hospital Stay | 1 Night | Usually Discharge on the Same Day |
| Recovery Time | 2 – 3 Weeks | 1 Week |
| Muscle Damage | Minimal | None |
According to Assoc. Prof. Dr. Erdinç Özek; “Another factor that is as important as the method in surgical success is the complete liberation of the nerve. Microsurgery and endoscopy are the most powerful tools that provide the surgeon with this precision. The important thing is to choose the one that best suits the patient’s anatomy.”
Postoperative Recovery Process
Thanks to modern surgical techniques, the healing process has accelerated considerably.
- Patients usually stand up and walk 4-6 hours after surgery.
- Heavy lifting and sudden turning movements should be avoided for the first 2 weeks.
- Patients can usually return to desk jobs by day 10 and light exercise by week 4.
Frequently Asked Questions
Does the hernia recur after surgery?
In cases where it is performed with the right technique and the patient pays attention to the postoperative lifestyle (weight control, exercise), the recurrence rate is below 5%.
Does hernia surgery leave paralysis?
Today, thanks to microsurgery and neuromonitoring technologies, the risk of nerve damage has decreased to almost non-existent levels.
Is laser hernia treatment the definitive solution?
Laser is not suitable for every type of hernia. It can only be used as an auxiliary method to reduce the pressure inside the disc in the initial, unruptured hernias.
Resource and Expert Knowledge
This article has been prepared in the light of Assoc. Prof. Dr. Erdinç Özek’s 2026 current literature data and minimally invasive surgery experiences in spine surgery. Assoc. Prof. Dr. Erdinç Özek is a senior surgeon with extensive case experience in microsurgical and endoscopic approaches in lumbar and neck hernias.