Stem cell transplantation from bone marrow is considered one of the most effective treatment methods for many serious blood diseases and types of cancer in today’s modern medicine.
This procedure is the process of replacing bone marrow cells that have lost their function or are damaged, with healthy and young stem cells.
According to Assoc. Prof. Dr. Erdinç Özek, stem cell transplantation is not just a cell exchange, but a reboot of the body’s defense and production mechanism.
What is Bone Marrow Stem Cell Transplantation?
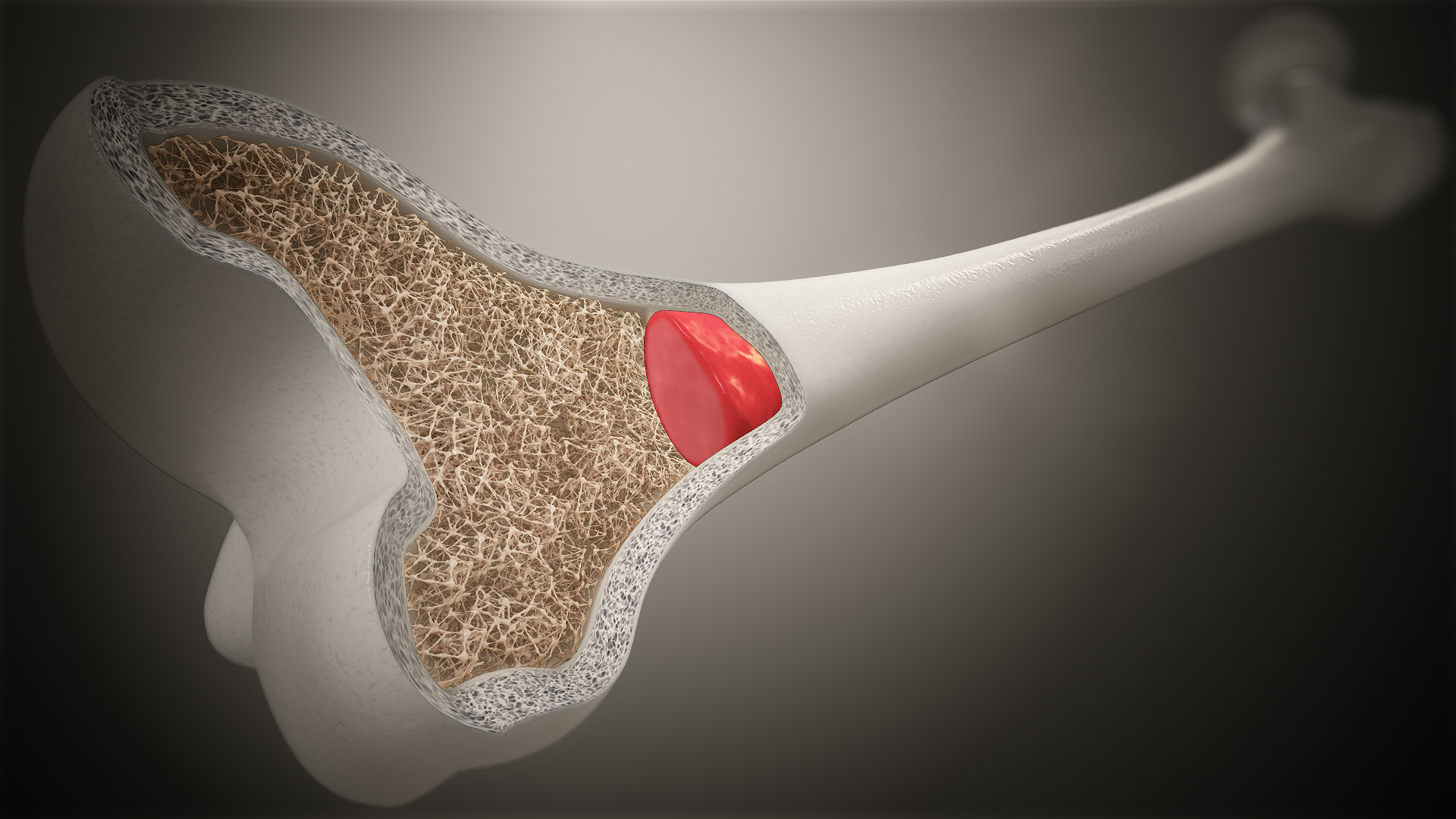
Bone marrow is a spongy tissue found in the central cavities of bones and is responsible for the production of blood cells.
Stem cell transplantation is the collection of “precursor” cells in this tissue and transferring them to the patient in need of treatment.
The Function and Importance of Bone Marrow in the Body
The bone marrow works like a blood factory of the body.
Billions of red blood cells (oxygen carriers), white blood cells (defense soldiers) and blood platelets (coagulation providers) are produced here every day.
If this factory starts to produce incorrectly or stops due to external factors, the vital functions of the body are at risk.
The Regenerative Power of Stem Cells and Their Therapeutic Role
Stem cells are the “parent” cells that have the ability to transform into all other cells in the body.
These transplanted cells have the power to settle in the patient’s bone marrow, restarting the production of healthy blood.
This regenerative power revitalizes the marrow that has been completely emptied after heavy chemotherapy or radiotherapy.
Which Diseases Is Bone Marrow Transplantation Used To Treat?
Stem cell transplantation may not be an option for every disease; However, in certain cases, this treatment is a life-saving necessity.
This method is generally used in cases that do not respond to standard treatments or have a high risk of recurrence.
Malignant (Cancer-Borne) Diseases and Transplantation Process
The main purpose of cancer-related transplants is to preserve the marrow after high doses of chemotherapy given to the patient.
The transplantation process is a critical stage in diseases such as leukemia (blood cancer), lymphoma (lymph node cancer) and multiple myeloma.
According to Assoc. Prof. Dr. Erdinç Özek, timing is the most important key to success in malignant diseases; The period when the cells are healthiest and the disease is suppressed is the best time for transplantation.
Hematological and Immune System Disorders
Not only cancers, but also diseases like aplastic anemia, where the bone marrow cannot produce blood, require transplants.
In addition, this method is frequently applied in children with Mediterranean anemia (thalassemia) and severe immune deficiency.
What are the Types of Stem Cell Transplantation from Bone Marrow?
When determining the type of transplant, the general condition of the patient, the stage of the disease and the presence of a suitable donor are the main criteria.
The following table can help you understand the key differences between transplant methods:
| Transplant Type | Source | Advantage | Risk Factor |
| Autologous | The patient himself | No risk of tissue rejection | Possibility of recurrence of the disease |
| Allogeneic | Fully matched donor | Establishes a new immune system | Risk of tissue rejection (GVHD) |
| Haploidentical | Semi-compatible relative | Possibility to find a donor quickly | Requires advanced expertise |
Autologous Transplant: Treatment with One’s Own Cells
In this method, the patient’s own healthy stem cells are collected before the disease progresses and stored by freezing.
After the high-dose chemotherapy process is over, these cells are returned to the patient.
Side effects are more limited because the body is not likely to reject its own cell.
Allogeneic Transplant: Cells from a Compatible Donor
If the disease does not allow using the patient’s own cells, cells are taken from a tissue-group-matched sibling or an unrelated donor.
The biggest strength of this method is the ability of the transplanted new cells to fight against cancer cells.
Haploidentical Transplant: The Semi-Compatible Transplant Option
In cases where a fully compatible donor cannot be found, it is a transplant from semi-compatible relatives such as mother, father or child.
Thanks to the developments in medical technology, very successful results can be obtained in this type of transplantation with special filtering methods.
According to Assoc. Prof. Dr. Erdinç Özek, haploidentical transplantation is one of the greatest opportunities offered by modern medicine for patients who do not have time to wait.
Clinical Experience Note (Anonymous Case):
A 45-year-old patient diagnosed with chemotherapy-resistant lymphoma underwent a semi-compatible (haploidentical) transplant when a fully matched donor could not be found. On the 21st day after transplantation, it was observed that the cells were attached and it was determined that the patient achieved a full cure (recovery) at the 1st year control.
How is Stem Cell Collection Performed from Bone Marrow?
The stem cell collection process is one of the most critical technical stages that determine the success of the transplant.
This procedure is a medical procedure that is meticulously planned according to the source of the cells and the patient’s condition.
Preparation Phase: Donor and Patient Evaluation
Before the cell collection procedure, the general health status of both the patient and the donor (donor) is checked through comprehensive tests.
Blood counts, infection screenings, and organ function tests are performed to confirm the safety of the process.
According to Assoc. Prof. Dr. Erdinç Özek, the slightest detail in the preparation phase directly affects the speed of adaptation of cells after transplantation.
Cell Collection from Bone Marrow in the Operating Room Environment
The traditional method of bone marrow collection is usually performed under general anesthesia in operating room conditions.
The required amount of marrow is aspirated by specialist physicians by entering from the back of the pelvis with the help of special needles.
This process takes about 1 to 2 hours and the collected marrow is passed through special filters and made ready for transplantation.
Recovery Process After Collection
The donor is usually monitored overnight after the procedure and discharged the next day.
It is normal to feel a slight ache or stiffness at the needle insertion sites, which may last for a few days.
The body completely renews these donated cells in about 2 to 4 weeks and brings them back to their former level.
How is Stem Cell Transplantation Applied? (Infusion Phase)
Contrary to popular belief, stem cell transplantation is not a surgical operation but an advanced blood transfusion procedure.
High Dose Chemotherapy and Radiotherapy Process
Before the cells are introduced, the patient undergoes an intensive treatment called a “priming regimen.”
The purpose of this process is to destroy diseased cells and make room in the bone marrow for new healthy cells.
Since this stage temporarily resets the immune system, it is vital to keep the patient in a fully sterile environment.
Transfer of Stem Cells to the Patient Intravenously
After the preparation process is over, the collected healthy stem cells are given to the patient through a central venous catheter.
The cells travel through the bloodstream to the bone marrow and begin to settle there in the nests reserved for them.
During this procedure, the patient is awake and the process is usually completed as simply as a serum transfer.
Post-Transplant Considerations and Recovery Period
The post-transplant period is a period of “attachment” that requires patience and very strict medical follow-up.
Retention Symptoms of Cells and Follow-up Process
When the given cells start to produce blood in their new homes, it is called “engraftment”.
Generally, an increase in blood counts between the 2nd and 4th weeks is the first sign that the cells are successfully attaching.
According to Assoc. Prof. Dr. Erdinç Özek, monitoring the patient’s temperature and daily monitoring of blood values during this period are the cornerstone of success.
Ways to Prevent Infection and Diet
Since the new immune system is not yet fully strengthened, the patient is vulnerable to the outside world.
Only well-cooked, fresh foods with low germ content should be consumed.
Visitor restrictions should be imposed and hygiene rules should be followed at the maximum level.
Dust, live flowers and pet contact should be avoided for a while in the home environment.
| Stage | Duration | Key Focus |
| Preparation Regimen | 7-10 Days | Clearance of diseased cells |
| Transplant Day | 1-4 Hours | Infusion of cells |
| Critical Wait | 14-21 Days | Attachment of cells to the marrow (Engraftment) |
| After Discharge | 6-12 Months | Reaching full capacity of the immune system |
Clinical Experience Note (Anonymous Case):
In a patient who underwent transplantation with the diagnosis of aplastic anemia, it was observed that the white blood cell count increased rapidly on the 14th day after transplantation. The patient’s full compliance with the isolation period of the first 100 days after discharge accelerated full recovery by reducing the possible infection risks to zero.
Frequently Asked Questions
Will donating harm my body?
No, stem cells are constantly renewed cells and the amount donated does not affect the health of the body.
What is the age limit to become a donor?
In Turkey, healthy individuals between the ages of 18-50 can generally be donor candidates.
Is the procedure very painful?
Since the collection in the operating room environment is performed under general anesthesia, no pain is felt during the procedure; Afterwards, there may only be a slight muscle ache-like ache.
Are only siblings checked for tissue compatibility?
First, siblings are screened, but if there is no compatibility, screening is done from unrelated national and international bone marrow banks.
Source and Expert Knowledge:
This content has been prepared with reference to Assoc. Prof. Dr. Erdinç Özek’s clinical experience and academic studies. Assoc. Prof. Dr. Erdinç Özek has many years of experience in the field of hematology and stem cell transplantation, and is a medical authority specializing in complex transplantation processes and cellular therapies.