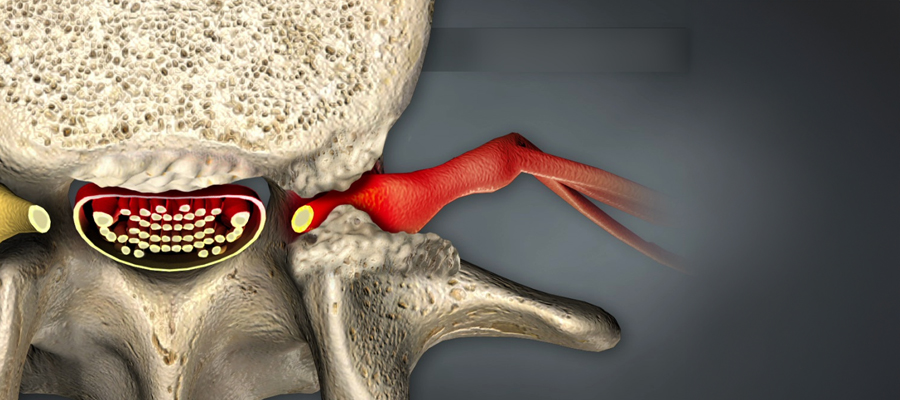
Deep Brain Stimulation (DBS), popularly known as “Brain Pacemaker“, is a surgical treatment method that regulates abnormal nerve signals by sending electrical impulses through electrodes placed at specific points in the deep structures of the brain.
This method is considered one of the most advanced solutions offered by neuromodulation technology for patients who do not respond adequately to medication or whose quality of life is impaired due to drug side effects.
What is Deep Brain Stimulation (Brain Pacemaker)?
Deep Brain Stimulation is an advanced system that regulates the electrical traffic inside the brain like an orchestra conductor.
Unlike traditional surgical methods, it has an adjustable and recyclable structure that does not cause permanent damage to brain tissue.
System; It consists of electrodes placed in the brain, a battery (IPG) placed in the chest area, and extension cables connecting the two.
How Does a Brain Pacemaker Work?
A brain pacemaker works by “resetting” or suppressing faulty electrical circuits inside the brain.
The abnormal signals emitted by neurons that are out of sync due to illness return to normal thanks to the controlled electrical current sent by the battery.
In this process, electrodes continuously send signals to the targeted area of the brain, while the doctor optimizes the intensity and frequency of this current according to the patient’s needs with the help of an external control.
According to Assoc. Prof. Dr. Erdinç Özek; “We should see the brain pacemaker not just as a device, but as a biological regulator that corrects the disrupted rhythm of the brain. The biggest advantage of the battery is that the treatment dose can be updated instantly with external programming as the patient’s clinical picture changes.”
In Which Diseases Is Deep Brain Stimulation Used?
Although Deep Brain Stimulation was initially used only for movement disorders, it is now evaluated in a wide range of neurological and psychiatric areas.
- Parkinson’s Disease: It is the most commonly used method to control symptoms such as tremors, stiffness and slowness.
- Essential Tremor: It shows high success in severe hand and body tremors that cannot be controlled with medication.
- Dystonia: It is preferred in posture disorders caused by involuntary contraction of muscles.
- Obsessive Compulsive Disorder (OCD): Surgery is offered as an option in advanced obsessive disorder.
- Epilepsy: It is used as an adjunctive therapy in suppressing foci resistant to other treatments.
The table below compares the key objectives of DBS implementation in different diseases:
| Type of Disease | Main Objective | Expected Recovery |
| Parkinson’s | Motor symptom management | Reduced tremor, freedom of movement. |
| Essential Tremor | Tremor control | Recovery of fine motor skills. |
| Dystonia | Muscle spasm reduction | Improvement in body posture and reduction in pain. |
| OCD | Circuit editing | Breaking the cycle of obsessive thoughts. |
Clinical Experience Note (Anonymous Case):
A 62-year-old patient who had been struggling with Parkinson’s for 10 years and developed severe involuntary movements (dyskinesia) due to medication underwent bilateral DBS. With the postoperative pacemaker settings, the patient’s drug dose was reduced by 50%, the tremors were almost completely controlled, and it was observed that the patient reached the capacity to eat alone.
Why is Deep Brain Stimulation (Brain Pacemaker) Performed?
Deep Brain Stimulation is performed to “restore quality of life” when standard drug treatments are no longer sufficient or when drug side effects make the patient’s life unbearable.
This treatment aims to reorganize the disrupted electrical rhythm in the depths of the brain, allowing the patient to perform daily tasks without being dependent on anyone else.
Although it does not completely eliminate the disease, it provides functional independence by dramatically reducing symptoms.
Parkinson’s Disease and DBS
In the treatment of Parkinson’s, DBS is used specifically to compensate for fluctuations between the “on-off” periods of medications.
It controls severe stiffness and inability to move during the periods when the effect of the drugs wears off, and involuntary movements (dyskinesia) during the periods when the drug dose is high.
Essential Tremor
Essential tremor is characterized by severe tremors, usually in the hands, that prevent the person from drinking or writing.
DBS can suppress these tremors by 80-90% by interfering with targets in the thalamus region of the brain, allowing the patient to return to his social life.
Dystonia
In dystonia patients, the brain sends a constant signal to the muscles to contract, resulting in abnormal postures and pain.
By interrupting these erroneous signals, DBS helps relax the muscles and bring body posture closer to normal.
Obsessive-Compulsive Disorder (OCD) and Other Uses
In psychiatric cases, DBS focuses on the areas of the brain that influence reward and mood cycles.
In severe cases of OCD resistant to medication and therapy, it breaks the cycle of obsessive thoughts and provides a significant improvement in the patient’s clinical picture.
Risks and Complications
As with any surgical procedure, Deep Brain Stimulation carries certain risks; however, these risks have been minimized with modern imaging and techniques.
The path to success is to share the risks transparently with the patient and to perform the operation in a fully equipped center.
Surgical Risks
The main risks that may be encountered during the surgical phase may arise during the placement of the electrodes.
- Brain Hemorrhage: Although it is very rare, it is a condition in which the vessels on the passageway of the electrodes are affected.
- Infection: They are inflammations that can occur in the surgical field or in the chest area where the battery is placed.
- Stroke or Neurological Losses: It is the risk of affecting sensitive areas during application.
Risks Related to Hardware and Programming
In the postoperative period, some disruptions may occur due to the technical parts of the system.
- Electrode Drift: Decreased effectiveness as a result of the displacement of the placed cables over time.
- Cable Breakage: Damage to extension cords passing under the skin as a result of excessive movement or trauma.
- Battery Life and Technical Errors: Temporary mood changes that occur during battery drain or programming.
The following table summarizes the risk profile and management strategies for DBS surgery:
| Risk Category | Possible Situation | Prevention/Management Strategy |
| Surgery | Infection | Sterile environment and use of prophylactic antibiotics. |
| Hardware | Battery Failure | Regular technical checks and periodic battery replacement. |
| Functional | Speech Disorder | Rearrangement of battery settings (frequency/current). |
According to Assoc. Prof. Dr. Erdinç Özek; “The most important safety layer in DBS surgery is the ‘microelectrode recording’ performed during surgery. In this way, it is 100% sure that the electrodes are in the right place and do not produce side effects while the patient is awake.”
Clinical Experience Note (Anonymous Case):
In a patient who developed speech impairment (lisping) in the postoperative period, it was determined as a result of the technical examination that this was not a surgical damage, but due to the high current of the battery. The pacemaker parameters were gradually optimized over a week, and the patient’s speech returned to normal while his tremors remained under control.
Preparation Process
The process after the decision for Deep Brain Stimulation is made is carried out with a meticulousness that directly affects the success of the surgery.
This stage aims to make the patient anatomically and psychologically most suitable for this advanced technological treatment.
According to Assoc. Prof. Dr. Erdinç Özek, the preparation process is not just about physical tests; Placing the patient’s expectations on a realistic basis is critical for the emotional success of the treatment.
Preoperative Evaluation and Tests
A multidisciplinary board evaluation is conducted to determine the patient’s suitability for surgery.
- Neurological Examination: The stage of the disease and the degree of response to medications (such as the UPDRS score) are measured.
- Imaging (MRI/CT): High-resolution imaging is performed to map the brain and determine the millimetric coordinates where the electrodes will be placed.
- Psychiatric Evaluation: It is checked whether the patient has mental health that can adapt to the post-operative process.
Nutrition and Medication Instructions
In the days before the surgery, some changes are requested in the patient’s routine.
While blood thinners are discontinued under the supervision of a doctor, it is generally requested not to take Parkinson’s medications on the morning of surgery (in order to better identify the target area in the brain).
Surgery Process (How is it Applied?)
Deep Brain Stimulation surgery is a high-tech surgery that usually consists of two main stages.
For the comfort and safety of the patient, every step is monitored with instant radiological and physiological data.
Neurosurgery Stage (Electrode Placement)
During this phase, the patient is usually kept awake; Because the surgeon wants to instantly test the effect of the placed electrode on the patient’s movements.
Under local anesthesia, electrodes are advanced through a very small hole drilled into the skull to the previously determined coordinates.
The “right point” is confirmed by talking to the patient or asking him to make simple movements; At this stage, the sudden cessation of tremors is the most impressive moment of the operation.
Chest Wall Surgery Stage (Battery Placement)
Once the electrodes are fixed, the patient is placed under general anesthesia.
The electrodes placed in the brain are connected to the battery unit, which is placed in a pocket opened in the chest area (under the collarbone) with the help of extension cables passed under the skin.
Postoperative Follow-up
The end of the surgery does not mean the end of the treatment; The real “fine-tuning” process begins now.
The healing process begins with the closure of surgical wounds, but the battery is expected to be activated for full functional gain.
Programming and Setting the Battery
Generally, the brain pacemaker is activated 2 to 4 weeks after surgery.
Using an external handheld terminal (programmer), the doctor optimizes the intensity, frequency, and width of the electrical current according to the patient’s symptoms.
These settings are updated several times over the following months to get the best results with the least dose of medication and side effects.
Things to Consider in Daily Life
Patients with a brain pacemaker can return to their normal lives to a large extent, but they should pay attention to some technical warnings.
Strong magnetic fields (such as some industrial devices) can interact with the battery.
In airport security passes and situations where MRI is required, it is vital to follow the appropriate protocols (such as MRI-compatible batteries) for the battery model.
The table below compares the stages of DBS surgery and patient experience:
| Stage | State of Consciousness | Duration | Basic Operation |
| Electrode Placement | Awake (Local Anesthesia) | 2 – 4 Hours | Brain mapping and electrode detection. |
| Battery Placement | Sleeps (General Anesthesia) | 1 Hour | Placement of the energy unit. |
| Programming | Uyanık (Polyclinic) | 30 – 60 Minutes | Setting of electrical parameters. |
Results and Expected Success Rates
Deep Brain Stimulation offers dramatic improvements in appropriately selected patients.
While increasing the daily “ten” (good movement) time by an average of 5-6 hours in Parkinson’s patients, it can reduce tremors by over 80%.
According to Assoc. Prof. Dr. Erdinç Özek; “Deep brain stimulation surgery is not an end, but a new beginning. Precise adjustments made during the first year after surgery are the main factor that makes that tremendous increase in the patient’s quality of life permanent.”
Clinical Experience Note (Anonymous Case):
In a 35-year-old patient who had difficulty walking due to severe dystonia before surgery, contractions decreased by 70% at 3 months after DBS. At the end of the first year, the patient started to walk independently without cane support, and thanks to the programmable structure of the battery, stabilization was achieved at a dose without side effects.
Frequently Asked Questions
Why do I need to stay awake during brain pacemaker surgery?
It is preferable to be alert so that the surgeon makes sure that he places the electrodes at the right point and tests your motor responses at that moment to observe side effects.
What is the lifespan of a brain pacemaker?
Depending on the type of battery used and the intensity of the electrical current, non-rechargeable batteries can serve for 3 to 5 years, while rechargeable batteries can serve up to 15 years.
Can those with a brain pacemaker have an MRI?
Most brain pacemaker systems produced today are “MRI compatible”; However, it is essential to set the battery to a certain mode before the procedure and to shoot with appropriate technical devices.
Does DBS treatment cure the disease completely?
A brain pacemaker does not eliminate the cause of the disease, but it significantly controls the symptoms and improves the patient’s quality of life to a much higher level than before surgery.
When does hair grow after surgery and when are stitches removed?
Recovery is fast because the incision sites are very small; The stitches are usually removed within 10-14 days, and the hair grows long enough to cover the surgical scars within a few weeks.
Is the brain pacemaker noticeable from the outside?
The electrodes on the head are completely under the skin; The battery in the chest area can only be seen as a slight swelling in very thin people, it is not visible from the outside.
Resource and Expert Knowledge
This guide is based on Assoc. Prof. Dr. Erdinç Özek’s surgical techniques in DBS operations and long-term postoperative patient follow-up protocols. Assoc. Prof. Dr. Erdinç Özek is a senior physician in Turkey who has the competence to transform technological opportunities in neuromodulation and brain pacemakers for the benefit of patients.