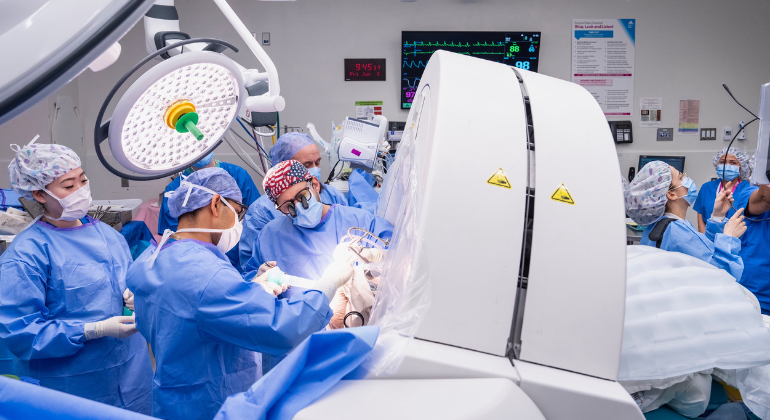
Endoscopic skull base surgery; It is a closed surgery method that uses natural holes (usually nasal passages) instead of opening the skull to reach complex areas at the base of the brain, accompanied by a high-resolution camera and sensitive devices.
This method offers a revolutionary approach in modern neurosurgery by allowing access to vital tissues, vessels and nerves at the bottom of the brain without external damage.
What is Endoscopic Skull Base Surgery?
Endoscopic skull base surgery is a minimally invasive discipline that uses the nasal cavity as a natural surgical corridor to treat tumors or structural disorders in the skull base.
While traditional open surgery requires large bone incisions (craniotomy) and brain tissue to be ruled out, the endoscopic method works with the principle of “inside out”.
The surgical team magnifies the anatomy at the base of the skull down to the smallest detail thanks to thin tubes called endoscopes, which have an ultra-high resolution (4K) camera with a cold light source at the end.
In Which Diseases Is Endoscopic Skull Base Surgery Applied?
This technique is successfully applied in many pathologies that are risky to reach by traditional means, especially those located in the center or base of the brain.
Pituitary Gland Tumors
Adenomas originating from the pituitary gland are one of the most common and successful areas where endoscopic surgery is performed.
By entering through the nose, the bone just below the pituitary gland (sella turcica) is opened and the tumor is cleaned without touching the brain.
Thanks to the high image quality, the border between the tumor and healthy pituitary tissue can be clearly distinguished, which helps to maintain hormonal functions.
CSF Leaks (Rhinorrhea)
It is a condition in which cerebrospinal fluid (CSF) flows out of the nose as a result of a bone defect or rupture of the membrane at the base of the skull.
With the endoscopic method, the hole that is the source of the leak is directly detected and repaired by occlusion with tissues (grafts) taken from the patient’s own body.
The success rate is much higher than open surgery, and the patient’s recovery period is significantly shorter.
Skull Base Tumors (Meningioma, Chordoma)
Complex masses such as meningioma, chordoma or craniopharyngioma located in the anterior, middle and posterior parts of the skull base can be treated with this method.
Especially in these tumors adjacent to the optic nerve (optic nerve) and the main carotid arteries, endoscopy offers the surgeon a wide viewing angle.
According to Assoc. Prof. Dr. Erdinç Özek; “Success in skull base surgery is not only to remove the tumor, but also to preserve the critical nerve structure and vascular network in that area. Endoscopy allows us to ‘see around the corner’, allowing us to remove tumor debris from blind spots that the microscope does not see. This is a vital advantage, especially in tumors with a high risk of recurrence.”
Clinical Experience Note (Anonymous Case): A 42-year-old patient presented with severe headache and inability to see the outer sides of both eyes (bitemporal hemianopsia). MRI examination revealed a large pituitary adenoma pressing on the optic nerves. The patient was operated endoscopically with a multidisciplinary approach (ENT and Neurosurgery). Immediately after the operation, the patient’s visual field was enlarged and the patient was discharged on the 3rd day because no intervention was made to the brain tissue.
How is Endoscopic Skull Base Surgery Performed?
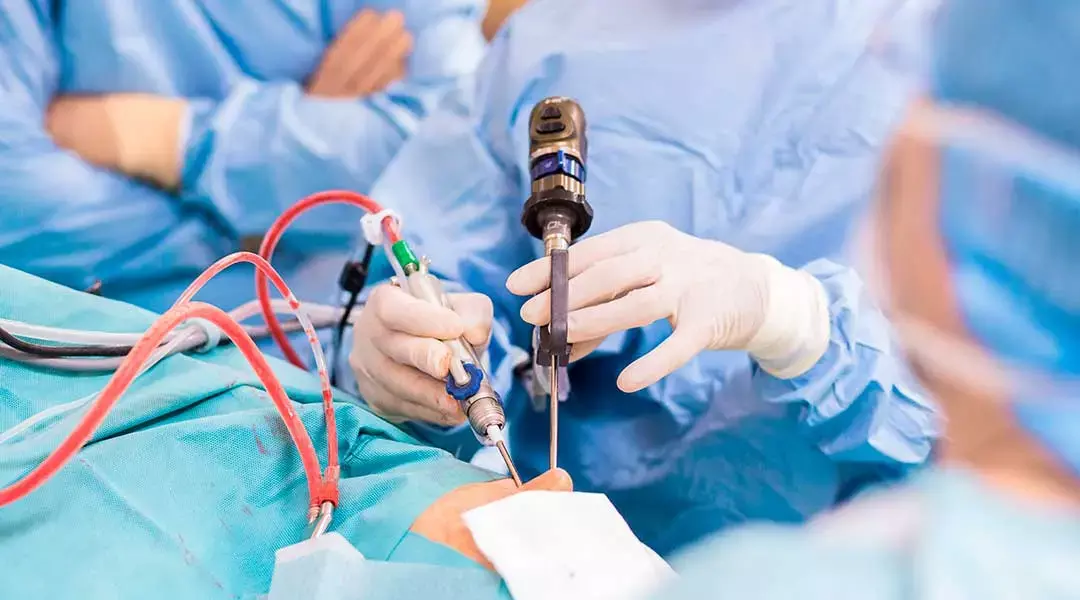
Endoscopic skull base surgery is performed with the “four-handed” technique, which requires millimetric precision and is usually performed by a Neurosurgeon and an ENT (Otorhinolaryngology) specialist.
- Preparation and Introduction: The surgery is performed under general anesthesia. By entering through the nostrils, the mucous structures are gently pulled aside and a corridor is created to reach the skull base.
- Navigation Setup: During the surgery, the “Neuronavigation” system, which allows the surgeon to see where he is in the brain to the millimeter, is activated. This acts as a surgical GPS.
- Opening the Skull Base: Depending on the location of the tumor, the thin bone structures at the base of the skull are opened with precision drilles (rasping devices).
- Tumor Removal: Accompanied by a high-resolution endoscope camera, the tumor is meticulously separated from the surrounding tissues (carotid artery, optic nerve, brainstem) and removed piece by piece.
- Closure (Reconstruction): After the procedure is finished, the most critical stage begins. Cerebral cortex (dura) and skull base; It is repaired watertight with tissues taken from the patient’s own nose (vascular flap) or medical adhesives.
What are the Advantages of Endoscopic Skull Base Surgery?
Compared to traditional open surgery, the endoscopic approach directly contributes to both the physical and psychological recovery process of the patient.
- Minimal Intervention to the Brain: Since there is no need to push the brain aside (retraction), the risk of edema or damage to brain tissue is much lower.
- No Scars Left Outside: Since the surgery is performed entirely through the nose, there are no incisions or stitches on the scalp.
- Wider Viewing Angle: While the microscope only sees a straight line, angled endoscopes allow the surgeon to “see the corners”, which makes it easier to remove hidden tumor fragments.
- Less Pain and Quick Discharge: Postoperative pain is minimal as large muscle incisions and bone valves are not opened; Patients can usually return home within 48-72 hours.
- Reduced Risk of Infections: Being a minimally invasive method, it reduces the risk of wound infection compared to open surgery.
Who is Suitable for Endoscopic Skull Base Surgery?
Not every skull base tumor may be suitable for the endoscopic method. The decision is made after a multidisciplinary board and radiological examinations.
- Those with Midline Tumors: They are the most ideal candidates for pituitary adenomas, chordomas and craniopharyngiomas.
- Those Experiencing CSF Leaks: Patients with brain fluid coming from the nose (rhinorrhea) are treated with high success with this technique.
- Those Who Cannot Tolerate Open Surgery: This less traumatic method may be preferred for elderly or poor general health patients.
- Those at Risk of Vision Loss: In masses that put pressure on the optic nerves, endoscopy is suitable to reach the nerve in the closest and safest way.
Assoc. Prof. Dr. Erdinç Özek; “The most important factor determining whether a patient is suitable for endoscopic surgery is the neighborhood relationship of the tumor with critical vessels and nerves. No matter how much our technology develops, sometimes the structure of the tumor may necessitate a combined approach with microsurgery (hybrid surgery). Our aim is to choose the ‘safest method for the patient’, not the ‘most modern’ method.”
| Feature | Endoscopic Surgery | Traditional Open Surgery |
| Incision Site | Inside the nose (No incision) | Scalp (Craniotomy) |
| Hospital Stay | 2 – 3 Days | 5 – 7 Days |
| Risk of Cerebral Edema | Minimal | Higher |
| Surgical Scars | Invisible | Prominent |
| Return to Normal Life | 1 – 2 Weeks | 4 – 6 Weeks |
Preoperative Preparation Process
Endoscopic skull base surgery requires a meticulous planning phase. The main purpose of this process is to optimize the surgical corridor (nasal passage) and to make an anatomical map of the tumor.
- Radiological Mapping: In addition to standard MRI, special “Thin Section CT” and “MR Tractography” shots are taken to be uploaded to the navigation device.
- Endocrinological Evaluation: If the tumor is a pituitary adenoma, the patient’s hormone levels are measured and, if necessary, preoperative hormone-regulating therapy is started.
- Multidisciplinary Examination: The neurosurgeon and the ENT specialist evaluate the nasal structure (deviation, sinusitis, etc.) together.
- Medication Management: Discontinuing blood thinners at least 7-10 days before surgery is critical for bleeding control.
Postoperative Recovery Process and Follow-up
From the moment the surgery is completed, the patient’s comfort and the preservation of the integrity of the skull base are at the forefront.
- Initial Observation: The patient usually spends the first night in the intensive care unit or intermediate care unit for neurological follow-ups.
- Nose Care: Tampons are usually not placed in the nose, but special sponges (nasal splints) that support tissue healing can be used.
- Activity Restriction: Heavy lifting, blowing your nose and straining-like movements that will increase intracranial pressure should be avoided for the first 2-4 weeks.
- Discharge: Patients are usually discharged on the 2nd or 3rd day, after checking for CSF leakage (water coming from the nose).
- Follow-up Period: The first check-up is done 1 week after the surgery. In the 3rd month, the first control MRI is taken to confirm the mass clearance.
Frequently Asked Questions
Will I experience loss of smell after surgery?
Modern endoscopic techniques focus on preserving the olfactory nerves. There may be a temporary decrease in odor, but the risk of permanent loss is quite low.
Is skull base surgery a risky surgery?
Every neurosurgical intervention has certain risks. However, the endoscopic method has significantly reduced complication rates because it does not rule out the brain and does not make external incisions.
What is the risk of brain fluid leakage (CSF)?
During surgery, the skull base is repaired with multi-layered techniques. In experienced hands and with the right repair methods, the risk of leakage has decreased to less than 1-3%.
Resource and Expert Knowledge
This content has been prepared in the light of the clinical foresight provided by Assoc. Prof. Dr. Erdinç Özek’s hundreds of successful operations on neuroendoscopy and skull base tumors and the medical literature for 2026. Assoc. Prof. Dr. Erdinç Özek is a senior surgeon in Turkey who advocates for a multidisciplinary approach to skull base surgery and specializes in minimally invasive techniques.