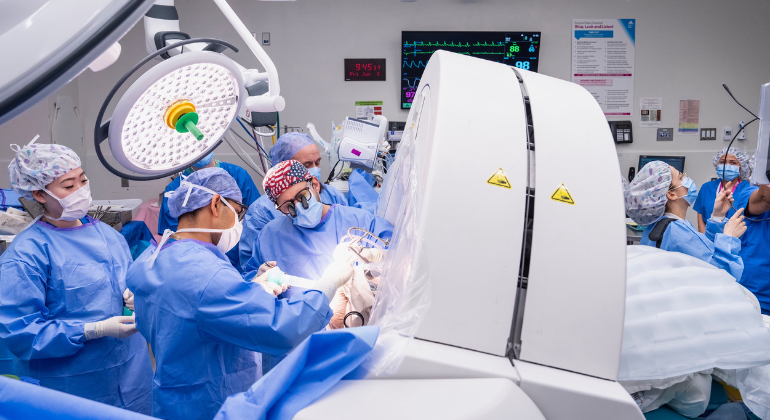
Functional neurosurgery; It is a branch of neurosurgery that treats diseases that occur as a result of deterioration of electrical or chemical functioning in the nervous system with advanced technological methods, even if there is no structural disorder in the brain tissue.
This surgical discipline aims to reorganize the patient’s impaired motor and sensory functions and improve their quality of life by intervening in specific areas of the brain (stimulation, modulation, or controlled lesion).
What is Functional Neurosurgery?
Functional neurosurgery is a field that focuses on the “working principle” of the brain rather than its anatomy.
While traditional neurosurgery usually focuses on removing “space-occupying” formations such as tumors or bleeding; Functional surgery focuses on regulating or suppressing nerve cells that are sending the wrong signal.
This branch, which is one of the most advanced points reached by modern medicine; It works with millimeter precision using neuromodulation techniques, microelectrode recordings and stereotactic methods.
Which Diseases Does Functional Neurosurgery Treat?
Functional neurosurgery comes into play in many neurological and psychiatric conditions where drug treatment is insufficient or its side effects cannot be tolerated.
Movement Disorders (Parkinson’s, Essential Tremor, Dystonia)
This group is one of the most common and successful areas of functional surgery.
- Parkinson’s Disease: Brain pacemaker (DBS) treatment is applied for symptoms such as tremor, stiffness and slowness of movement that cannot be controlled with medication.
- Essential Tremor: In hand and head tremors that end the patient’s social life, 80-90% improvement is aimed with interventions in the thalamus region of the brain.
- Dystonia: In this disease, which causes involuntary contractions in the body, overactive nerve circuits are surgically modulated.
Epilepsy (Epilepsy) Surgery
In drug-resistant epilepsy patients, the frequency and severity of seizures are reduced by surgical removal of the focus where seizures begin or by stimulation of nerve pathways (such as VNS).
Spasticity Treatment
In severe muscle stiffness (spasticity) that develops after stroke, MS or brain injury, the patient’s mobility is increased by placing Baclofen pumps that secrete drugs into the spinal cord.
Chronic Pain and Trigeminal Neuralgia
In cancer pain or persistent pain due to nerve damage, operations such as spinal cord pacemakers (SCS) or microvascular decompression of the trigeminal nerve, which prevent pain signals from reaching the brain, are performed.
Psychiatric Disorders (Obsessive Compulsive Disorder)
In severe and untreatable cases of OCD, functional interventions that regulate the limbic system of the brain can be considered as a last resort according to current protocols.
According to Assoc. Prof. Dr. Erdinç Özek; “Functional neurosurgery is the surgery to ‘give the life back’ to the patient. For example; The fact that a Parkinson’s patient who cannot hold his spoon can eat alone after a brain pacemaker is not only a medical achievement, but also a great functional gain. However, it should not be forgotten that; These surgeries aim to reduce the symptoms to the most manageable level rather than completely returning the patient to ‘normal’.”
| Disease Group | Main Symptom | Preferred Surgical Method |
| Parkinson’s | Tremors, slowness of movement | Deep Brain Stimulation (DBS) |
| Epilepsy | Resistant Seizures | Focal Resection or VNS |
| Spasticity | Severe Muscle Stiffness | Baclofen Pump |
| Chronic Pain | Neuropathic Pain | Spinal Cord Pacemaker (SCS) |
Methods Used in Functional Neurosurgery
Functional neurosurgery is the field where technology is integrated with medicine at the highest level.
These methods work by reprogramming the brain’s electrical networks or regulating nerve conduction through biochemical means.
Deep Brain Stimulation (Deep Brain Stimulation – DBS)
Brain pacemaker is the most accepted surgical method worldwide for Parkinson’s and tremor disorders.
- System: It consists of thin electrodes placed in the nuclei deep in the brain and a battery unit placed in the chest area.
- Mechanism: The battery sends continuous and adjustable electrical impulses to the brain, suppressing the erroneous signals that cause symptoms.
- Advantage: It is a reversible method; It does not cause permanent damage to the natural tissue of the brain and can be adjusted externally with the help of a computer.
Baclofen Pump Applications
It is especially used to manage severe spasticity that develops after cerebral palsy or spinal cord injury.
- System: It is a pump with a drug reservoir placed under the skin in the abdomen.
- Mechanism: The drug (Baclofen) is delivered directly into the spinal fluid (intrathecal space) through a thin catheter.
- Advantage: It provides much more effective results at much lower doses than taking the drug orally; This minimizes systemic side effects.
Vagal Nerve Stimulation (VNS)
It is a “nerve pacemaker” method used in cases of drug-resistant epilepsy.
- Application: An electrode is wrapped around the Vagus nerve in the neck area and the battery is placed in the rib cage.
- Impact: It sends signals to the brain at regular intervals, reducing the frequency and severity of seizures.
Lesion Surgery (Radiofrequency Thermocoagulation)
It is an older but still used method of targeted permanent intervention in certain cases.
- Application: It is the deactivation of a millimeter nerve focus that causes pain or tremors by means of heat, using radiofrequency energy.
- Reason for Preference: It is generally preferred in patients for whom battery replacement is risky or who do not want implants.
Recovery Process After Functional Neurosurgery Surgery
These surgeries require a sensitive follow-up process as well as high technology.
- Hospital Stay: After brain pacemaker and similar procedures, patients are usually discharged within 2-3 days.
- Battery Setting (Programming): Approximately 2-4 weeks after DBS surgery, “battery opening” is performed. Several adjustments may be required in the first months for the patient to reach the best level of motor function.
- Sewing and Hygiene: The incisions in the head and chest area heal in about 10 days. During the recovery period, the area should be protected against the risk of infection.
- Return to Social Life: Patients can usually fully return to their routine social and work lives 1 month after surgery.
Assoc. Prof. Dr. Erdinç Özek; “In functional surgery, surgery is only half the way. The other half is the precise battery programming to be done after surgery. Each patient’s brain map and electrical needs are different. Therefore, communication between the physician and the patient should be kept very tight for the first year after surgery.”
| Method | Application Area | The Most Common Disease | Persistence Status |
| Deep Brain Stimulation (DBS) | Brain Nuclei | Parkinson’s, Tremor, Dystonia | Adjustable / Reversible |
| Baclofen Pump | Spinal Canal | Spasticity | Drug Focused / Programmable |
| Nerve Pacemaker (VNS) | Vagus Nerve | Refractory Epilepsy | Automatic Stimulator |
| Radiofrequency | Target Nerve Focus | Pain, Trigeminal Neuralgia | Permanent / Targeted |
Clinical Experience Note (Anonymous Case):
In a 62-year-old male patient who had been treated for Parkinson’s for 15 years, DBS was planned after the residual drugs caused the “on-off” phenomenon. With the postoperative battery adjustments, involuntary movements (dyskinesia) that make the patient’s daily life difficult were reduced by 70%. While the patient could not dress without preoperative help, he reached the level where he could walk alone 3 months after the procedure.
Frequently Asked Questions
What is the lifespan of a brain pacemaker?
Depending on the model and energy level used, batteries typically last between 3 to 5 years; There are also models that can be charged externally and have a lifespan of 15-25 years.
Is it mandatory to be awake during brain pacemaker surgery?
Traditionally, the patient is kept awake for microelectrode recording; however, today, thanks to advanced imaging techniques, “asleep DBS” operations are also successfully performed.
What happens if spasticity pump dies?
It gives an alarm before the pump runs out. The medication reservoir is easily refilled with an external injection without the need for surgical procedure.
Resource and Expert Knowledge
This content has been prepared based on Assoc. Prof. Dr. Erdinç Özek’s current clinical achievements in advanced neuromodulation and stereotactic surgery techniques in 2026 and neurosurgery application protocols. Assoc. Prof. Dr. Erdinç Özek is a competent specialist in the surgical management of complex movement disorders and functional diseases.