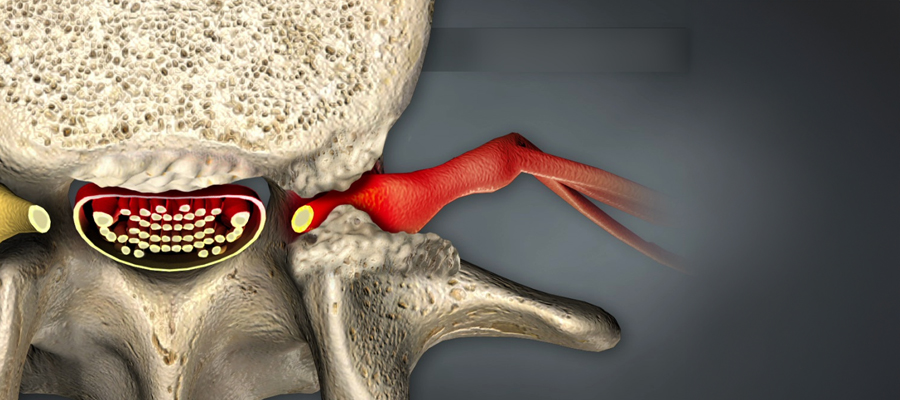
Nerve compression or entrapment neuropathy with its medical name; It is a condition in which the peripheral nerves passing through certain parts of the body lose their function by being exposed to physical pressure in the narrow canals or anatomical tunnels they pass through.
This condition not only disrupts the electrical conduction of the nerve, but can also cut off the blood flow that feeds the nerve, leading to permanent damage to nerve fibers and muscle wasting in the long term.
What is Nerve Compression (Entrapment Neuropathy)?
Nerve compression is when the peripheral nervous system, our body’s intricate electrical network, encounters a mechanical barrier.
It passes through the nerves, muscles, tendons and bones in our body and reaches the target tissues.
If these passageways (tunnels) are narrowed due to trauma, edema, structural defects or constantly repetitive movements, the nerve is “trapped” in this area.
The trapped nerve becomes unable to transmit the correct signals to the brain, causing both sensory and motor (movement) losses.
What are the Symptoms of Nerve Compression?
Although the symptoms of nerve compression vary depending on which body part the compressed nerve serves, they generally follow a similar course.
The most common clinical signs are:
- Numbness and Tingling: A “pinprick and needles” sensation occurs in the fingers or skin area, which is usually stimulated by the affected nerve.
- Pain: It is pain that starts from the compression area and spreads along the nerve, sometimes burning and sometimes felt as an electric shock.
- Loss of Strength (Muscle Weakness): In advanced stages, weakening begins in the muscles dominated by the nerve. For example; situations such as not being able to hold an object in the hand or tripping the foot are observed.
- Symptoms That Increase at Night: Especially in wrist impingements, patients often state that they wake up at night with numbness and pain.
- Muscle Wasting (Atrophy): In very prolonged and severe compression, a noticeable decrease in muscle mass occurs, which usually indicates a stage that is difficult to reverse.
According to Assoc. Prof. Dr. Erdinç Özek; “Many patients delay consulting a doctor, mistaking the numbness in their hand for simple fatigue. However, nerve compression is a ‘race for time’. The longer the pressure on the nerve lasts, the less the nerve’s ability to repair itself. Especially if weakness or wasting has started in the muscles, it may be too late for surgical intervention. Taking the symptoms seriously early on is the only way to prevent permanent damage.”
What are the Most Common Nerve Compressions?
Our body has many narrow tunnels through which nerves pass between bones, ligaments and muscles. Narrowing in any of these tunnels leads to a specific impingement syndrome.
Carpal Tunnel Syndrome (Nerve Compression in the Wrist)
The most common entrapment is neuropathy. It is the pressure of the Median nerve , which passes through a narrow canal in the wrist.
- Symptom: Numbness in the first three fingers and half of the fourth finger, night pains and dropping objects from the hand.
Ulnar Nerve Compression (Cubital Tunnel Syndrome)
It usually occurs in the elbow area, in the area known as the “funny bone”.
- Symptom: Numbness in the little finger and ring finger, weakness in the inner small muscles of the hand and the appearance of a “claw hand” in the advanced stage
Peroneal Nerve Compression (Nerve Compression in the Knee Area)
It occurs on the outer side of the knee, at the level of the fibula bone head.
- Symptom: It is the inability to lift the foot up and loss of sensation in the upper part of the foot, known as “drop foot”.
Tarsal Tunnel Syndrome (Nerve Compression in the Ankle)
It is the compression of the tibial nerve in the tunnel on the inside of the ankle.
- Symptom: It creates burning, tingling and a feeling as if there is a fold in the sock on the sole of the foot.
Meralgia Paresthetica (Nerve Compression in the Thigh Area)
It is the compression of the nerve that receives the sensation of the outer thigh (Lateral femoral cutaneous nerve) in the groin area.
- Symptom: It is burning, numbness and tenderness on the outer side of the thigh; It usually does not cause movement disorders, only sensory loss.
What Causes Nerve Compression? What are the Risk Factors?
Nerve compression is rarely due to a single cause; It is usually caused by a combination of structural predisposition and environmental factors.
- Repetitive Movements: Computer use, continuous use of hand tools or some sports (tennis, etc.) increase the pressure in the tunnel.
- Metabolic Diseases: Diabetes lowers the resistance of nerves to pressure. Hypothyroidism and rheumatoid arthritis also trigger impingement through edema.
- Pregnancy: The increased fluid retention in the body can lead to temporary but severe compression, particularly in the carpal tunnel area.
- Anatomical Structure: In some individuals, the tunnels through which the nerves pass are congenitally narrower.
- Traumas: Fractures, dislocations or hard blows to the area can narrow the nerve pathway.
According to Assoc. Prof. Dr. Erdinç Özek; “Especially when we look at our patients with ulnar nerve compression, we see that the habit of working with their elbows resting on hard surfaces is a trigger. A simple lifestyle change (elbow brace or table ergonomics) can save a beginner patient from the operating table. However, if we cannot eliminate the risk factors, the success of the surgery may be overshadowed.”
| Syndrome Name | Jamming Zone | Affected Area | Critical Risk Factor |
| Carpal Tunnel | Wrist | First 3.5 Fingers | Keyboard work, Diabetes |
| Cubital Tunnel | Elbow | Last 1.5 Fingers | Elbow against hard ground |
| Peroneal | Next to the knee | Back of the Foot | Crossing your legs for a long time |
| Meralgia Paresthetica | Groin | Outer Thigh Side | Excess weight, Use of narrow belts |
How is Nerve Compression Diagnosed? (EMG and Imaging)
The most critical step in the diagnosis of nerve compression is the overlap of the patient’s history and physical examination. However, objective tests are needed to determine the degree and exact position of the print.
- EMG (Electromyography): It is the “gold standard” of nerve compression diagnosis. It measures the electrical conduction speed of nerves. It clearly reveals where the conduction in the nerve slows down and whether damage has started in the muscles.
- Ultrasonography (USG): It allows us to see the thickening (edema) in the area where the nerve is compressed and the pressure of the surrounding tissues (cyst, tumor, etc.) live.
- MRI Imaging: It provides anatomical detail, especially in cases that may be confused with neck and lumbar hernia or in the suspicion of a formation occupying space in the tunnel.
Nerve Compression Treatment Methods
The treatment plan is determined according to the severity of the damage to the nerve. In mild cases, conservative (non-surgical) methods are prioritized.
Non-Surgical Treatments and Medication Use
In mild and moderate compression, it is aimed to reduce the pressure on the nerve and resolve edema.
- Splint Usage: Especially in the carpal tunnel, night splints that keep the wrist in a neutral position reduce intracanal pressure.
- Medication: B vitamins (for nerve repair), anti-inflammatory drugs that dissolve edema and neuropathic painkillers are used.
- Injections: Cortisol or PRP injections into the canal can provide temporary or permanent relief by reducing local edema.
- Physical Therapy: With nerve gliding exercises, the mobility of the nerve in the tunnel is increased.
Surgical Intervention (Nerve Release Surgeries)
Surgery is essential in patients who are severely damaged on EMG, muscle wasting has started, or do not respond to 3-6 months of non-surgical treatment.
- Microsurgical Release: Under the operating microscope, the thickened ligament or bony protrusion that compresses the nerve is completely cut and the nerve is “liberated”.
- Technique: In this procedure, which is performed with very small incisions (approximately 2-3 cm), even the thin membrane (neurolysis) on the nerve is cleaned and blood flow is revived.
Recovery Process After Nerve Compression Surgery
Thanks to modern surgical techniques, patients can be discharged on the same day and quickly return to their daily lives.
- First 24 Hours: Postoperative pain is minimal due to the effect of local anesthetics. Patients may start moving their hands or feet slightly.
- Dressing and Stitches: The incision area should not be in contact with water for 10-14 days. Since aesthetic stitches are usually used, there is no hassle of removing stitches.
- Speed of Recovery: The pain usually goes away immediately after surgery. However, it may take several months for the numbness to go away, as it is related to the rate at which the nerve regenerates itself (about 1 mm per day).
- Return to Work: Those who work in desk jobs can work at full capacity within 3-5 days, and those who work in jobs that require heavy physical strength can work at full capacity after 4-6 weeks.
Assoc. Prof. Dr. Erdinç Özek: “The most common sentence we hear from our patients after surgery is ‘That heavy burden on my hand has been lifted’. Surgery removes pressure on the nerve in seconds, but it takes patience for the nerve to heal at the cellular level. Not smoking in this process (as it disrupts nerve blood supply) and not interrupting the recommended exercises can double the recovery rate.”
Clinical Experience Note (Anonymous Case): In a 52-year-old tailor patient, “severe carpal tunnel” was detected in EMG performed with the complaint of severe numbness and inability to hold scissors in both hands. After the relaxation performed by microsurgical method, the patient’s pain that woke him up at night was completely relieved from the first night. It was observed that he completely regained his fine motor skills (such as needle and thread) 1 month after the operation.
Frequently Asked Questions
Do complaints recur after nerve compression surgery?
The recurrence rate in relaxation surgeries performed with the correct technique is below 1%. Recurrence is usually seen in cases where the nerve is not fully relieved or excessive scar tissue (scar) forms in the area.
I have pain even though my EMG test is normal, what should I do?
Sometimes there may be situations that we call “negative EMG”; that is, the jamming is very recent and has not yet been reflected in the transmission speed. In this case, diagnosis can be made with clinical examination and USG and treatment can be started.
What happens if I don’t have surgery?
If the pressure continues, the fibers within the nerve begin to die. This leads first to persistent numbness and then to paralysis (wasting) of the muscle group involved. Unfortunately, surgeries performed after this stage cannot bring back the dead fibers.
Resource and Expert Knowledge
This article is based on Assoc. Prof. Dr. Erdinç Özek’s current clinical achievements in 2026 on peripheral nerve microsurgery, EMG correlation in the diagnosis of entrapment neuropathies, and neurolysis techniques. Assoc. Prof. Dr. Erdinç Özek is an expert who applies advanced surgical approaches to the preservation and restoration of nerve health.