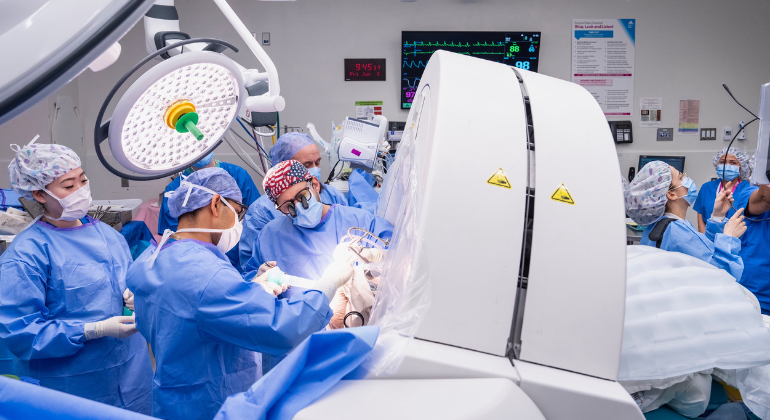
Vagal Nerve Stimulation (VNS), also known as the “Vagus Pacemaker”, is a biological treatment method that regulates brain activities by sending low-intensity electrical currents to the vagus nerve, one of the longest and most important nerves in the body.
This method modulates the electrical traffic on the nervous system, especially in neurological and psychiatric disorders resistant to medication, allowing symptoms to be controlled.
What is Vagal Nerve Stimulation (VNS)?
Vagal Nerve Stimulation is an advanced medical procedure that affects the brain’s neurotransmitter balance by stimulating the vagus nerve through a generator (battery) and electrodes.
This procedure, which is performed over the vagus nerve, which is seen as the “insurance of the body” in modern medicine, is a dialogue between the battery placed in the rib cage with the nervous system with a surgical intervention.
VNS is an effective non-invasive neuromodulation technique that aims to improve brain function through a peripheral nerve without directly interfering with brain tissue.
What is the Vagus Nerve and Where Is It?
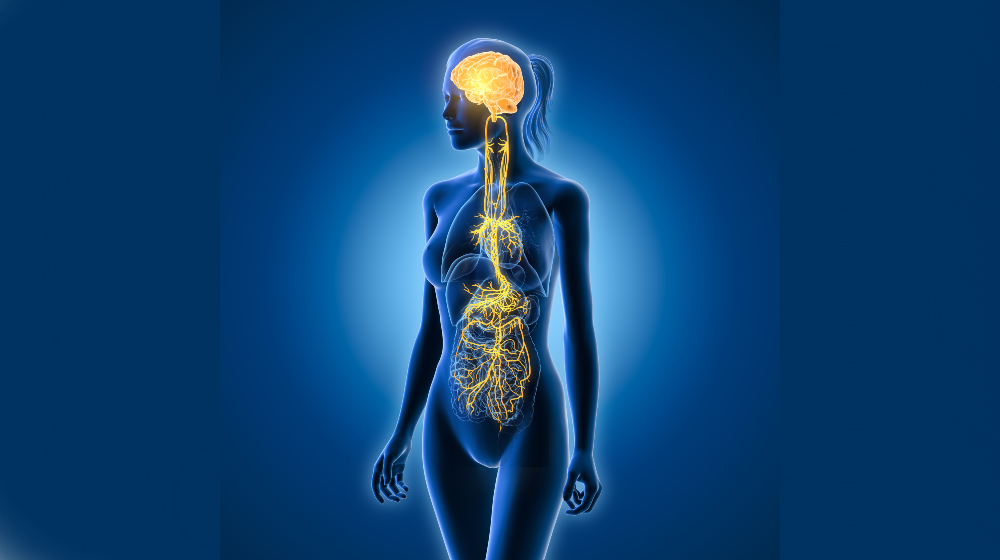
The vagus nerve is the tenth most complex cranial pair in the body (10th cranial nerve), extending from the brainstem to both sides of the neck to the chest and abdominal cavity.
The word “vagus” means “wanderer” in Latin; The name comes from the nerve’s extensive spread, connecting many vital organs such as the heart, lungs, and digestive system.
The vagus nerve, located on the left side of the neck, is usually preferred as part of the treatment, as its effect on heart rhythm is much more limited than the right side and is the safest way for stimulation.
According to Assoc. Prof. Dr. Erdinç Özek; “The vagus nerve is the largest information highway between our brain and body. With VNS treatment, we regulate the ‘faulty traffic’ on this highway and open a new door of control in challenging conditions such as epilepsy, to which the brain resists.”
How Does a VNS Device (Vagus Battery) Work?
VNS system; It consists of a small metal generator placed under the chest, electrodes wrapped around the nerve, and a programmer device.
The system sends electrical signals to the brain over the vagus nerve at certain time intervals determined by the doctor (for example, 30 seconds of warning, 5 minutes of waiting).
These signals are distributed to different parts of the brain through nuclei in the brainstem, suppressing the overstimulation of neurons and helping to restore chemical balance.
The following table summarizes the working principles and components of a VNS system:
| Component | Function | Technical Detail |
| Generator (Battery) | Generates electric current | It is placed under the skin in the chest area. |
| Electrode Wire | Transmits the signal to the nerve | It wraps around the left vagus nerve in the neck. |
| Magnet | Provides manual control | When a seizure is felt, it triggers extra stimulation from the battery. |
Clinical Experience Note (Anonymous Case):
A 40% reduction in seizure frequency was observed in the first 6 months after VNS administration in a 22-year-old patient who had seizures an average of 15-20 times a month and did not respond to 3 different antiepileptic drugs. It has been reported that the patient can stop many seizures before they start thanks to the “hand magnet” he uses when he feels that seizures are coming.
Why is Vagal Nerve Stimulation Performed?
Vagal Nerve Stimulation is applied to regulate the electrical activity of the brain and stabilize neural conduction pathways.
It aims to control severe attacks or mood disorders that reduce quality of life by offering a surgical alternative for patients who do not respond to medication.
Refractory Epilepsy (Epilepsy) and VNS
In about one-third of epilepsy patients, medications are insufficient to stop seizures.
By suppressing abnormal electrical discharges in the brain, VNS reduces the frequency, duration, and severity of seizures.
Shortening the recovery time after seizures is one of the most obvious gains of this treatment on patients.
Treatment-Resistant Depression
In severe cases of depression, standard antidepressants and psychotherapies may not always yield results.
VNS sends continuous stimulation to brain regions that regulate mood through the vagus nerve, helping to restore neurotransmitter balance in these areas.
Other Potential Uses
In recent years, research shows that VNS has shown promise in other areas due to its anti-inflammatory effects.
Clinical studies are ongoing on the effect of vagal stimulation in conditions such as migraines, cluster headaches, inflammatory bowel diseases and Alzheimer’s.
Who is a Suitable Candidate for VNS Treatment?
VNS is not the first choice for every patient, but rather an advanced line treatment that is considered for patients who meet certain criteria.
- Refractory Epilepsy: Patients whose seizures cannot be controlled despite using at least two or three different antiepileptic drugs in appropriate doses.
- Suitability for Surgery: People who are not suitable for brain surgery (focus removal) or who have not benefited from this surgery.
- Refractory Depression: Patients over the age of 18 with chronic and recurrent depression that does not improve despite multiple treatment methods.
According to Assoc. Prof. Dr. Erdinç Özek; “The most critical point in VNS candidacy is the correct selection of the patient. If the patient feels that his seizures are coming (aura period), he is in the group that benefits the most from VNS, as he has the chance to stop the seizure before it starts thanks to the hand magnet.”
Risks and Complications
Vagal Nerve Stimulation is a procedure that is generally considered safe; However, as with any surgical procedure, some side effects may occur.
These risks are usually temporary and can be controlled by adjusting the battery’s settings.
Risks Associated with the Surgical Procedure
These risks, which are associated with the surgery itself, are very low.
- Infection: It can be seen in the chest area or neck incision area where the battery is placed.
- Vocal Cord Damage: Since the vagus nerve is close to the vocal cords, there is a risk of temporary hoarseness during surgery.
- Nerve Irritation: Sensitivity of the nerve during the placement of the electrodes.
Stimulation (Device Operation) Related Side Effects
These effects usually occur when the battery is active (sending alerts) and decrease over time.
- Hoarseness or Voice Change: It is the most common side effect; It only happens when the battery is active.
- Sore Throat and Cough: A tickling sensation may occur in the throat during stimulation.
- Shortness of Breath: If stimulation comes during physical activity, a temporary shortness of breath may be felt.
The following table summarizes the management of VNS side effects:
| Side Effect | Seen Time | Solution Method |
| Hoarseness | When sending a battery alert | Lowering the current strength (mA). |
| Cough | First weeks | Adjustment of signal frequency. |
| Skin Allergy | After surgery | Appropriate dressing and medical treatment. |
Clinical Experience Note (Anonymous Case):
In a teacher patient who experienced hoarseness while speaking after VNS insertion, the on-time stimulation time of the battery was shortened and the current was gradually increased. In this way, the body was accustomed to the stimuli, and at the end of the 3rd month, there was no voice problem affecting the patient’s social life.
Preparation Process
The decision to undergo Vagal Nerve Stimulation is a strategic decision made considering the patient’s lifestyle and current treatment history.
The main goal at this stage is to create a roadmap that will maximize surgical success while minimizing possible side effects.
According to Assoc. Prof. Dr. Erdinç Özek, the preparation process is the first and most important step of the patient’s long-term relationship with the battery.
Preoperative Evaluation
Before the surgery, the patient’s general health status and neurological picture are examined comprehensively.
- Vvideo-EEG Monitoring: In epilepsy patients, the character of seizures and the possible benefit from the pacemaker are analyzed.
- Cardiological Control: Since the vagus nerve is associated with heart rhythm, the patient’s heart health is tested for suitability for this procedure.
- Psychosocial Preparedness: Realistic expectations are created by explaining in detail how the device will work and the use of magnets to the patient.
Medication and Food Instructions
There are certain medical protocols that the patient must follow before undergoing surgery.
On the day of surgery, the doses of antiepileptic drugs are usually adjusted as recommended by the doctor and it is requested to comply with the required fasting period for the stomach cavity.
Supplements or medications with blood thinning effects should be discontinued under the supervision of a doctor for a certain period of time (usually 1 week) before surgery.
How is Vagus Pacemaker (VNS) Surgery Performed?
Vagus pacemaker surgery is an operation that takes less time and has a high recovery rate compared to neurosurgery standards.
The procedure is usually performed under general anesthesia, but local anesthesia options may also be considered depending on the patient’s condition.
Placement of the Device and Electrodes
The surgical process is carried out simultaneously with the intervention in two different parts of the body.
First, the vagus nerve is found through a small incision made in the left neck area and special electrode wires are precisely wrapped around the nerve.
In the second stage, a “pocket” is created in the upper part of the left rib cage (in the area near the armpit) and the battery generator is placed in this area.
Electrodes are connected to the battery unit through tunnels passed under the skin and the electrical integrity of the system is tested on the operating table.
Postoperative Follow-up and Programming
The postoperative period is divided into two as “adjustment” and “adaptation”.
Once the integration of the device into the body is complete, the programming process customized to the patient’s clinical needs begins.
Commissioning and Setting the Device
The battery is activated, usually 2 to 4 weeks after surgery, when the surgical sutures have completely healed.
The doctor adjusts the battery’s current strength (milliamps), warning time and standby time via a wireless tablet or computer.
As the patient’s body gets used to the stimulation, these doses are gradually increased at follow-up appointments to reach the most ideal treatment level.
Magnet Usage and Function
One of the most unique features of the VNS system is the manual control it provides to the patient.
When patients pass a special magnet attached to their wrist or belt over the battery, they send an “extra warning” command to the system.
When this method is used at the moment when the seizure is felt to start (aura period), it can stop the seizure, shorten its duration or reduce its severity.
Results and Expected Success Rates
VNS treatment is a method that shows its effect cumulatively (increasingly) over time.
There is a high proportion of patients who see a 50% reduction in seizures within the first year of treatment; However, this success rate can reach up to 60-70% in the second and third years.
The table below compares the effects of VNS therapy on patients over time:
| Process | Expected Development | Quality of Life Impact |
| 0 – 3 Months | Getting used to the system and adjusting the dose | Reduction of side effects (hoarseness, etc.). |
| 3 – 12 Months | Gradual reduction in seizure frequency | Optimizing drug doses (if possible). |
| 1 Year + | Maximum clinical benefit | Increased participation in social life and alertness. |
According to Assoc. Prof. Dr. Erdinç Özek; “VNS is not just a seizure preventer; It is also a life support system that increases the patient’s mental alertness and accelerates the recovery process after a seizure. Most of our patients state that they feel much more energetic even if their seizures are not completely over.”
Frequently Asked Questions
Is vagus pacemaker surgery risky?
It is a very low-risk procedure compared to general surgical procedures; The rate of serious complications is very low because it is worked only under the skin in the neck and chest area without interfering with the brain tissue.
How long does a VNS battery last?
The life of the battery varies between 5 and 10 years on average, depending on the current intensity applied and the model of the battery; When the energy level decreases, the battery unit is replaced with a short procedure performed under local anesthesia.
Does the use of magnets completely stop the seizure?
Although the magnet does not cut the seizure like a knife in every patient, in most cases it reduces the severity of the seizure, shortens its duration and helps the patient to recover cognitively much faster after the seizure.
Is hoarseness a side effect permanent damage?
No, hoarseness is usually a temporary condition that only occurs within seconds when the device sends an alert; With sensitive updates to the battery settings, this side effect is reduced to a level that does not disturb the patient.
Can a patient with a vagus pacemaker have an MRI?
Most current VNS devices are MR-compliant under certain security protocols; However, a physician’s control is absolutely necessary to turn off the battery or bring it to the appropriate mode before shooting.
Is the surgical scar very visible from the outside?
Since the incisions in the neck and chest area are made with the principles of plastic surgery, they become indistinct over time; Since the scar on the neck is usually hidden in the natural neck lines, it does not cause any obvious discomfort in terms of aesthetics.
Resource and Expert Knowledge
This article was written with reference to Assoc. Prof. Dr. Erdinç Özek’s clinical research on VNS surgery, battery life monitoring, and neuromodulation outcomes. Assoc. Prof. Dr. Erdinç Özek is a pioneer in technical precision and long-term patient management in VNS applications in Turkey